Having a new baby at home goes hand in hand with high stress, sleepless nights, lots of self-doubt and even more learning. When it’s two babies, expect all of that in spades. And how about when one of those babies came straight from a five-month stint in the NICU? Dizzying doesn’t even describe it.
Avery was released from the hospital April 12, 153 days after she was born and more than three months after her twin brother, August, got his walking papers. Their homecomings were both eagerly anticipated but have rolled out very differently. August—who was born at about 3 pounds, nearly triple his sister’s birth weight–quickly grew by leaps and bounds (tipping the scale at 13.5 pounds now), started sleeping (mostly) through the night early on and is smashing through his milestones for his adjusted age. Avery’s transition has been a bit more complex—just like she has been from day one—riddled with doctor’s appointments, therapies, an influx of medical supplies in our living room and an immensely steep learning curve.
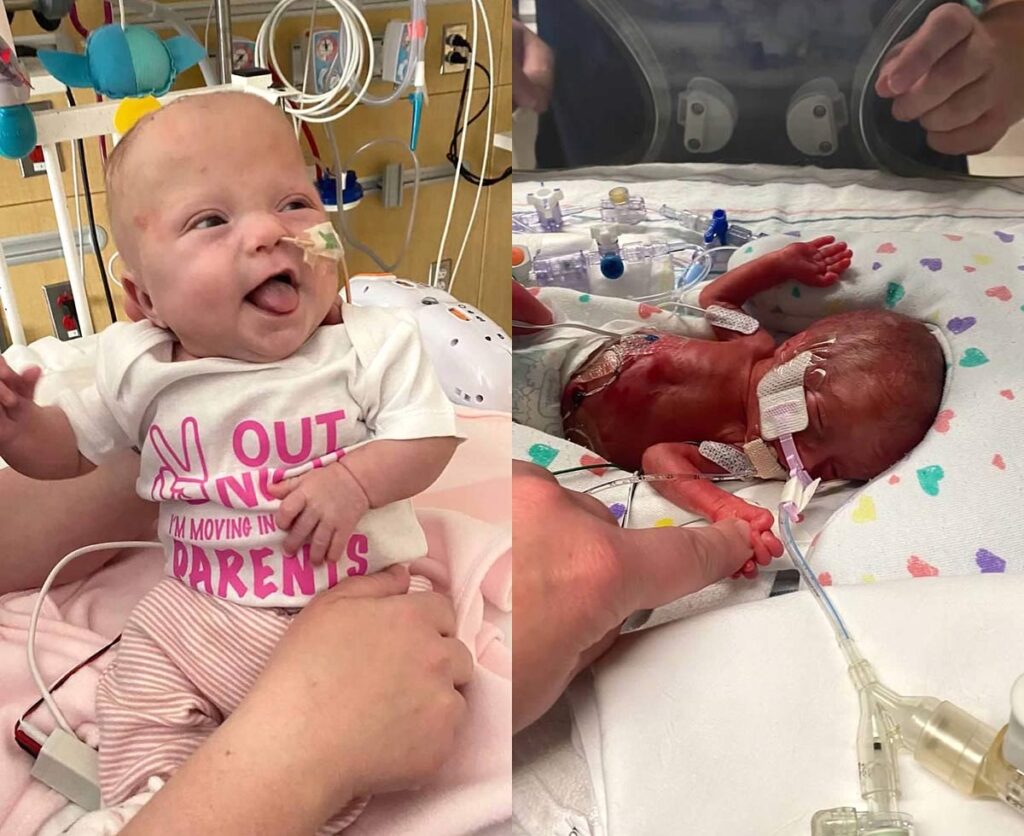
From the NICU to the living room
When August was discharged from the NICU in January, he largely left the monitors, wires and medications behind him. Instead, he filled our house with the usual baby refuse: diapers, wipes, bibs, burp cloths and swaddles–all of varying degrees of cleanliness! When it was Avery’s turn, however, the clutter was ratcheted up a few notches.
On top of diagnoses including hydrocephalus and pulmonary hypertension, she left the hospital with a nasogastric (NG) feeding tube in her nose, as she’s struggled to learn bottle feeding. That means her bassinet in our living room is surrounded by an IV pole carrying a feeding bag and an electric pump, while the diaper carrier attached is brimming with tube supplies, including a stock of three different types of tape to secure the tube to her face and pH strips to test the placement in her stomach, while what used to be Jackson’s high chair n the kitchen is now the home of her overflow NG supplies.
Though we felt well-trained to care for her NG tube, we were nonetheless nervous, and her first day home did nothing to quell those fears. As we pulled into our driveway from the hospital, Avery yanked the tube out of her nose, leading to a chaotic homecoming where we were tripping through the five months of belongings from the hospital we haphazardly threw across the living room as we scrambled to replace the tube for the first time ourselves. She’s since pulled it out several times and, while we’re getting slightly more used to the extremely unpleasant task of holding her down and threading the tube through her nose and into her stomach (props to my new nursing school grad wife for taking the lead on this one most times!). The NG tube is one of the banes of our post-NICU existence.
While our house often feels like a clinical setting now, Avery also has plenty of actual medical appointments to go to. Later this month, she’ll be back in the hospital to say sayonara to her NG tube for a surgical placement of a G tube in her belly. Since her release, she’s had two brain scans, a hip ultrasound, bloodwork and seen the neurologist (twice), nephrologist, NICU outpatient clinic, nutritionist, feeding therapist, physical therapist and pediatrician (many times!).
On one recent pediatrician appointment, I was feeling particularly proud of getting the twins into the car and to the office by myself (and on time!). I had successfully set up Avery’s feeding bag and pump for an on-the-go feed but, as I was unloading her car seat into the twin stroller, I got sprayed in the face with milk–and realized I had caught her NG tube on the car door, yanking it out of her nose during her feed, a major no-no (risk of aspiration) I remembered from my NG training. Thankfully, the pediatrician’s office staff was well-versed in dealing with panicked parents like myself!
Complications and caution
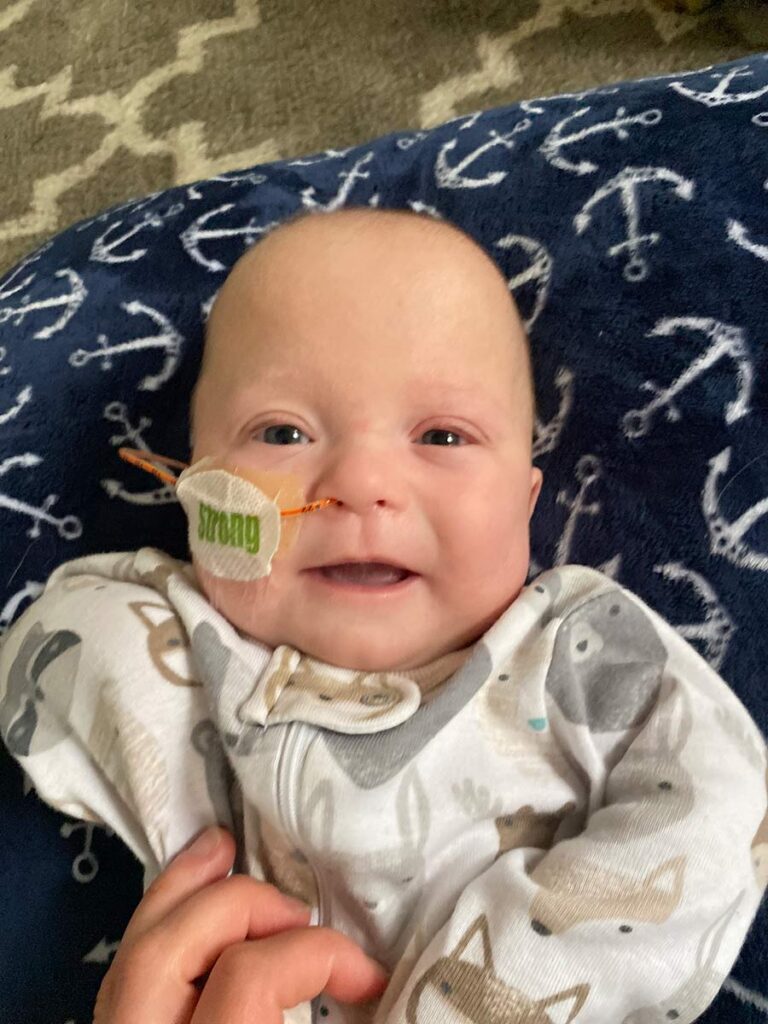
That situation highlighted a reality most NICU parents likely face when their baby comes home: Every little decision we make when it comes to Avery seems like it could bring about the end of the world. She was on the brink for so long that our minds were trained to appreciate the gravity of every single nuance that goes into keeping her alive — and now, it’s totally our responsibility. So, when the pediatrician shared that, even though she wasn’t actively aspirating from losing her NG mid-feed, we’d have to watch for signs of aspiration over the next 12 hours. I was an absolute mess and felt like the world’s worst parent.
Logically, of course I know I’m not. But when you have a medically complex baby in your care, any little deviation from her norm can be a pretty big deal, which means we’re constantly questioning and second-guessing ourselves. Nearly all parents likely have that mentality to some degree: Is the bath water too hot? Is it OK to let the baby cry for a few minutes to grab a quick shower? What if this formula isn’t right for their stomach? But with a baby who spent her entire life in the NICU, it feels like there’s no room for mistakes, no room for us as parents to give ourselves a little grace to mess up.
For the first few weeks of her being home, we had to feed her every three hours. If we were even a few minutes late we entered into a panic. She gets medicine five times a day, and each time we double-check, it has to be precisely the right dose, drawn up with no bubbles. When we put her milk into her feeding bag, we’re often crunching numbers like accountants to ensure we’re giving her the right volume at the right rate. And while August was also a NICU baby, his lack of significant complications has made his post-care world different than Avery’s: Any time a family member babysat him since he got home, we’d essentially pre-fill a few bottles and say, “Feed him when he’s hungry and keep him alive — thanks!” Avery had her first sitters last weekend for about five hours, and I wrote out a mini novel to make sure they were in step with her complex care.
Learning a new balance

One of the biggest worries Ashlee and I had when we found out we were having twins was the impact it would have on our 3-year-old, Jackson — long used to being the center of attention! We eased him into big brotherhood when we brought his brother home two months after his birth and started learning the art of paying attention to two kids despite constant distractions. Enter a third kid with significant medical needs and we’re forever feeling like we’re being pulled in competing directions (sometimes literally!).
A 3-year-old demands A LOT of attention and, though I’ve struggled at times to dole that out to Jackson’s liking while being a full-time remote worker and part-time stay-at-home mom, I’ve been pretty proud of how I’ve challenged myself to be present for him. But lately, I’ve said the phrases “Hold on,” “I can’t right now,” “Be right there,” and “When I’m done with your sister” more times than I would like.
NICU or not, any parent of multiples can probably relate to the feeling of having to triage who needs you most at the moment: Who’s crying louder? Who’s hungrier? Who’s likely to pitch the bigger fit? And with a kid with a medical history longer than a CVS receipt, it’s tempting to always put Avery at the top of the priority list. Though she hasn’t even hit 10 pounds yet, she seems to carry more weight than her older brothers — so, we’re still trying to find a balance that lets us meet her needs without making her NICU experience our driving focus.
The NICU is not just a bad memory for parents; it’s a living memory that shapes all aspects of a family’s life. Bringing a baby home is supposed to be a time for parents to find their footing but, with a post-NICU baby, it feels like that footing is about to be kicked out from underneath you at all times because the baby came into the world under so much uncertainty. So, this new chapter is not actually “new” — it’s an extension of the one that came before it. And it’s certainly a wild ride.
