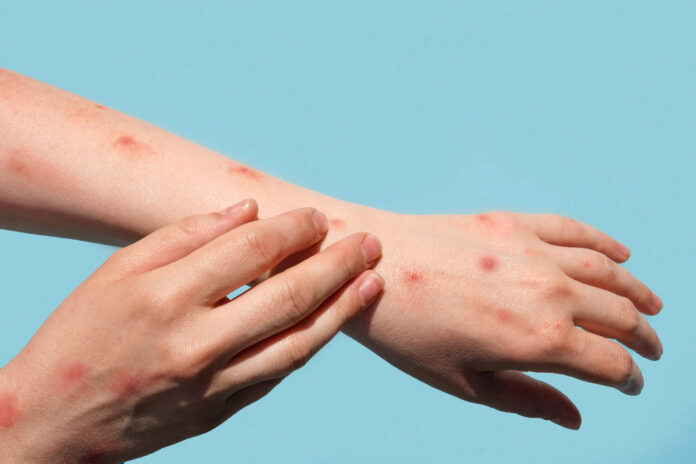
Monkeypox is spreading – globally, throughout the U.S. and in Philadelphia. As PGN reported, the virus already meets the criteria for a pandemic.
As of July 19 there are 14,945 confirmed cases globally with Spain (3,359), Germany (2,110), and the U.K. (2,137) reporting the highest case counts.
The U.S. has 2,108 reported cases as of July 19, with the highest numbers in New York, California and Illinois. Pennsylvania has 64 recorded cases, 33 of which are in Philadelphia.
But all these numbers have been rising significantly on a weekly basis. The Center for Infectious Disease Research and Policy (CIDRAP) reported July 18 that the opportunity to control monkeypox in the U.S. has been missed and that the reported cases in no way reflect the volume of actual cases.
Former Obama Food and Drug Administration (FDA) commissioner Scott Gottlieb, MD, said on July 17 that the window for controlling monkeypox in the U.S. has probably closed and said the official U.S. total of confirmed cases is only a small fraction of the cases in the country.
“I think they’re going to be reluctant to use the word pandemic, because it implies that they’ve failed to contain this, and I think at this point we’ve failed to contain this,” Gottlieb told CBS “Face the Nation” moderator Margaret Brennan. “We’re now at the cusp of this becoming an endemic virus, with this now becoming something that’s persistent that we need to continue to deal with.”
“I think the window for getting control of this and containing it probably has closed, and if it hasn’t closed, it’s certainly starting to close,” he added.
Cases have primarily been detected among men who have sex with men, but Gottlieb says the virus has “spread more broadly in the community.” He told Brennan that the reports have come mostly from sexual health clinics. “We’re probably detecting just a fraction of the actual cases,” he said.
Kaiser Health News notes that “vaccine and testing delays for monkeypox echo failures in early COVID response” and quote gay men citing their frustration with the lack of available vaccine and testing.
Into this fraught arena the Philadelphia Department of Public Health (PDPH) announced July 19 that it has received its first shipment of JYNNEOS vaccine for monkeypox. The PDPH said it will “begin administering it to people who are at high-risk of becoming infected. These doses will be administered, by appointment only, to people who have been identified as contacts of people who have confirmed or probable monkeypox and others considered at high-risk.”
“Monkeypox is a rare, but potentially serious infection that is preventable,” said Coleman Terrell, the Health Department’s director of Disease Control. “Philadelphia has recently been allocated doses of vaccine that can help protect those who may have been exposed to monkeypox. We believe that with a targeted distribution strategy, we can help contain the outbreak and continue to protect those in our community.”
The Health Department has received 1,605 doses of JYNNEOS vaccine, which is indicated for smallpox and monkeypox, for distribution. An additional 1,020 doses are expected to be received during the week of July 25, 2022. These vaccines will be made available to people who are considered to be high-risk at invitation-only clinics at a Health Department site.
In a statement to PGN, the PDPH noted, “due to the relatively small number of vaccine doses available, eligibility to receive the vaccine is limited to people who have been identified as contacts of people who have tested positive for monkeypox and those identified by the Health Department as being at high risk. As more doses become available, the Health Department will continue to expand the vaccine program.”
Erik Larson, Deputy Director of the Office of LGBT Affairs, said, “At this time, we are focused on protecting and treating those who are at the highest risk for exposure, and letting equity guide our decision-making process.“
Larson added, “as we wait for more doses of vaccine to become available from the federal government, we encourage individuals to make safer personal choices where possible. Although monkeypox isn’t considered an STI, we always encourage individuals to have open conversations with their partners in order to increase safety and mitigate risk.”
Dr. Mark Watkins, a physician at Mazzoni Center, told PGN, “Mazzoni Center has been actively testing patients for monkeypox. The number of patients contacting the office with monkeypox questions has been increasing significantly recently, which is a cause for concern.”
“Patients are aware of this recent health threat,” Watkins said. “Symptoms have ranged from mild rash to larger pox outbreaks as well as oral lesions to significant anal pain requiring pain medications. There is a medication available through compassionate use accessible from the CDC called tecovirimate. So far patients have been tolerating this medication extremely well with limited side effects and a good response.”
Watkins added that “It is expected within this week that a broader vaccination effort will be starting. This will include Mazzoni Center as a vaccination site for patients.”
Patients usually first experience symptoms like fever, headache, muscle aches, chills, exhaustion and swelling of the lymph nodes.
Within one to three days after initial symptoms, infected individuals develop a rash that typically spreads from the head to other parts of the body. The incubation period for the disease can be as long as three weeks.
The PDPH also launched a new blog post that provides advice for people who may have been exposed, and for those who may be experiencing symptoms of monkeypox. If a person is exposed to someone with monkeypox, they should call the Health Department at 215-685-5488 immediately. The Health Department will ask about the exposure and work with that person to set up an opportunity to receive a vaccine to help keep from getting monkeypox.
The Health Department emphasized to PGN that “the vaccine must be provided as soon as possible, so making this call quickly is important. Vaccine is being distributed first to those at the highest risk, so people who may be lower-risk might not get an immediate vaccine appointment. People who are experiencing symptoms of monkeypox are encouraged to contact their regular healthcare provider, and tell their partners, as soon as possible. People who are experiencing symptoms of monkeypox or have been diagnosed with monkeypox cannot be vaccinated.”
One of the problems facing health care providers was cited in the PDPH statement, that for the time being, the Health Department, similar to other health agencies worldwide, will only provide one dose of the monkeypox vaccine per eligible person.
“This means that, while the vaccine requires two doses to be considered fully vaccinated, people won’t be immediately scheduled for their second dose and may not receive it at the recommended 28-day interval,” the PDPH statement reads.
PDPH added, “research has shown that this delay should not negatively affect the immune response given by the second dose. This is the best way to ensure that as many people as possible get at least one dose. As more vaccine becomes available, the Health Department will work to contact those who need a second dose.”
The Department of Health and Human Services (HHS) announced an additional 2.5 million doses had been purchased and would be entered into the Strategic National Stockpile (SNS) in early 2023. The purchase brings the federal government’s available supply of vaccine to treat monkeypox to nearly 7 million doses by mid-2023 – a full year from now.
Since late May when cases began to spread, HHS made more than 300,000 doses available to states and territories.
The EU has secured only 54,000 doses of the monkeypox vaccine and delivered around 25,000 doses to six member states, according to Reuters.
For the latest information about the outbreak, visit the CDC website.